Carotid artery disease
Carotid stenosis: what are the risks and treatment options? Carotid stenosis is a narrowing of the carotid artery, most often linked to atherosclerosis. Its main risk is neurological: fragments of plaque or a clot can migrate to the brain and cause a transient ischemic attack (TIA) or a stroke. Why can carotid stenosis be dangerous? The carotid arteries carry a large portion of the blood destined for the brain. When an atherosclerotic plaque develops, it can reduce the diameter of the artery but, more importantly, become a source of embolisms to the cerebral circulation, which exposes the patient to a TIA, a full-blown stroke, sometimes permanent after-effects, and more rarely, death. The risk is not the same for all patients. It depends in particular on whether the stenosis is symptomatic or not, the degree of narrowing, the stability of the plaque, and the patient’s overall cardiovascular profile.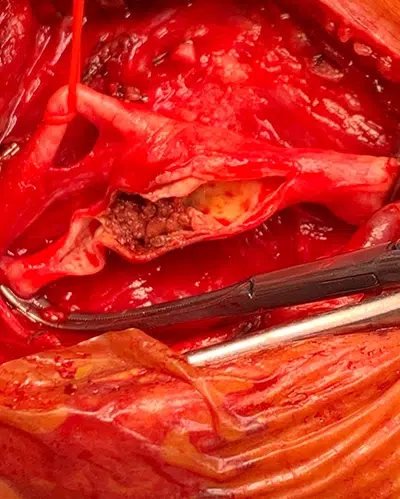

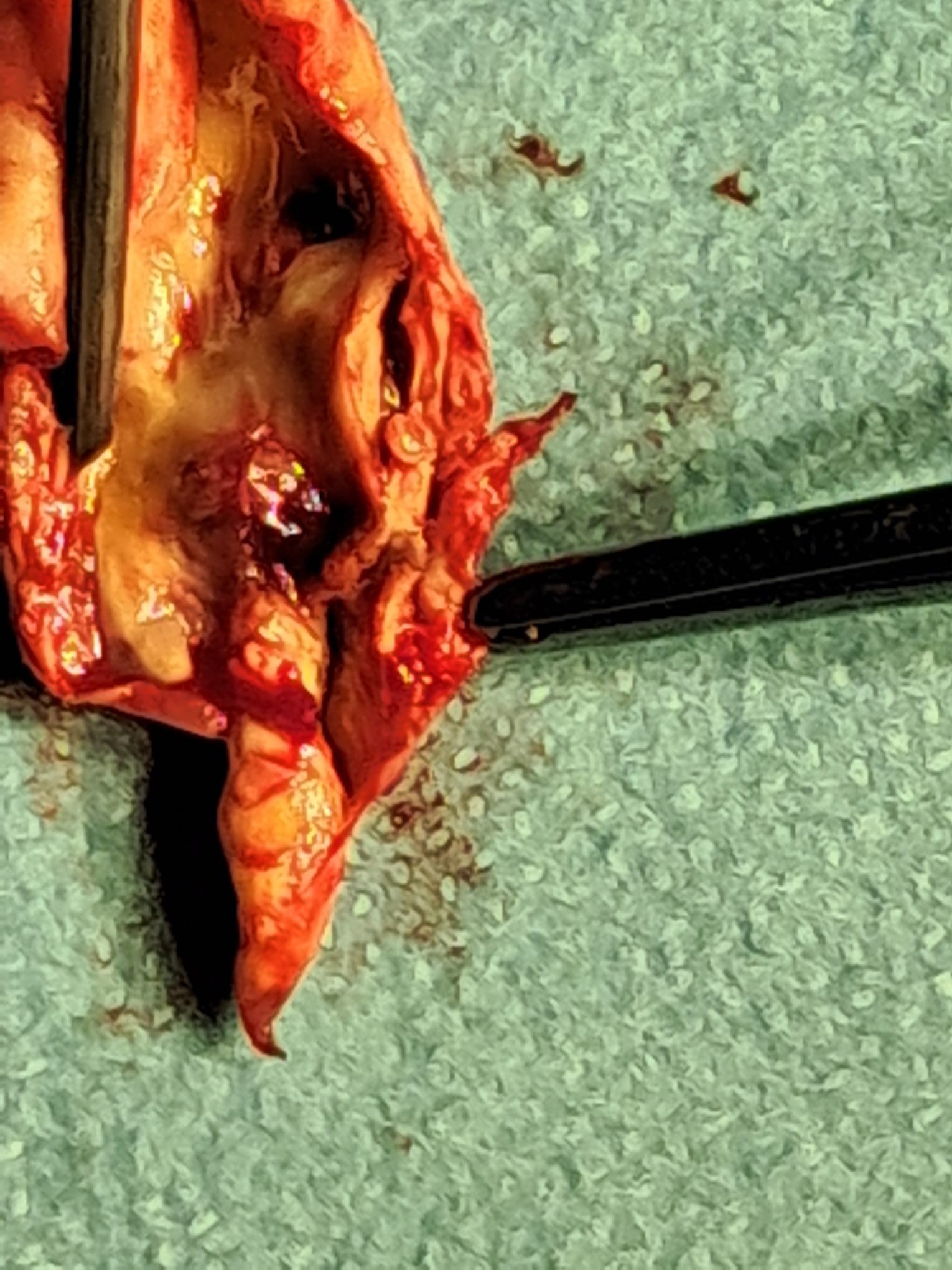
What symptoms should raise concern?
What symptoms should raise concern?
What are the treatment options?
Intensive medical treatment is essential for all patients, regardless of whether intervention is decided upon. It is based on strict blood pressure control, taking antiplatelet therapy as indicated, high-intensity statin therapy or appropriate lipid-lowering therapy, smoking cessation, physical activity, diabetes management, and correction of other cardiovascular risk factors.
When stenosis is symptomatic, or when asymptomatic stenosis is deemed high-risk in a specialized setting, revascularization may be considered. The two main techniques are carotid endarterectomy, which involves surgically removing the plaque, and carotid stent angioplasty , which aims to treat the narrowing endovascularly.
The 2023 European guidelines emphasize that the decision must be individualized according to symptoms, anatomy, age, surgical risk, comorbidities, and the expertise of the surgical team. They also reiterate that the historical 30-day risk thresholds remain at 3% for asymptomatic patients and 6% for symptomatic patients, thus necessitating rigorous selection of indications.
What the CREST-2 study shows
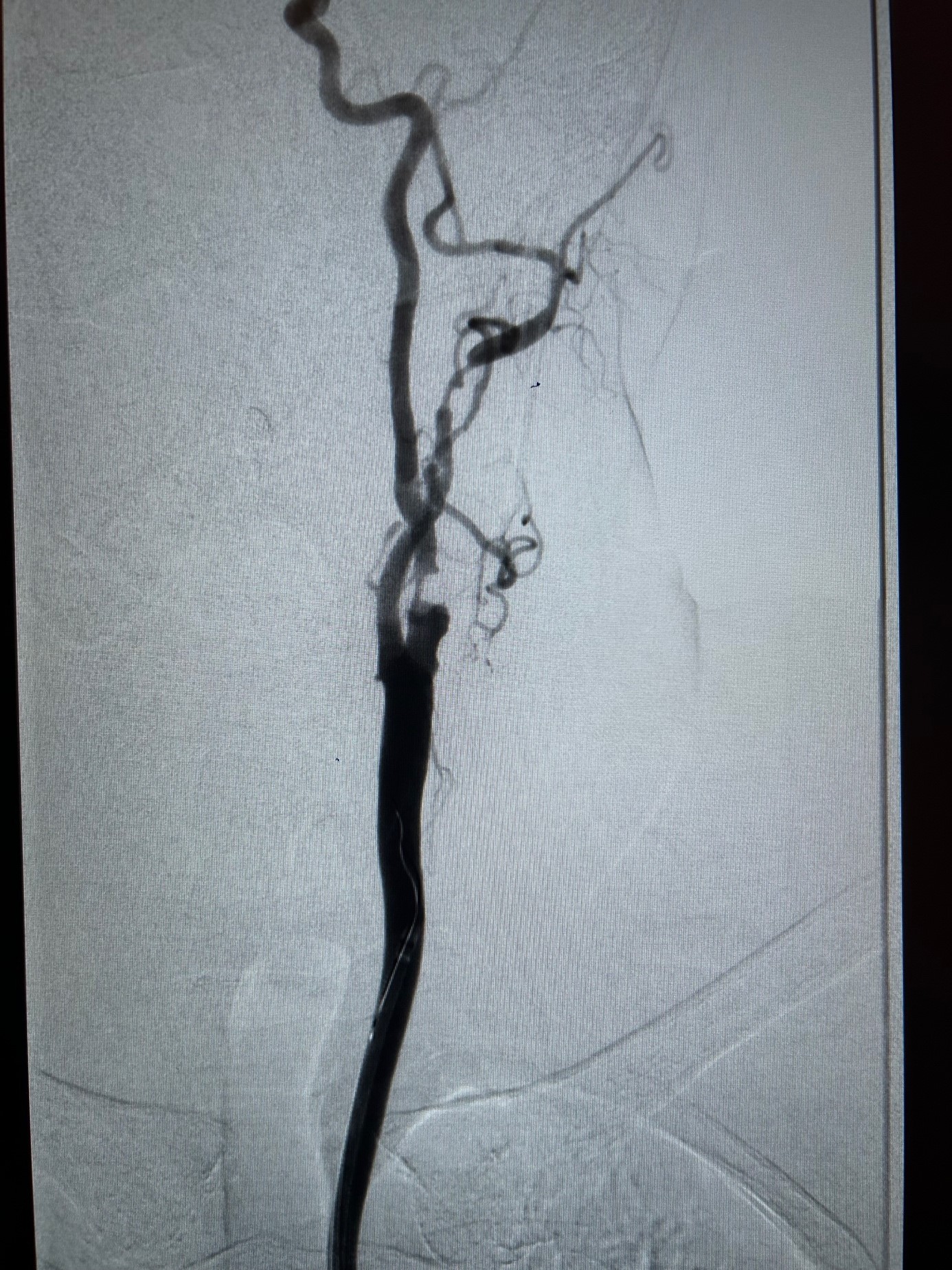
Visualization of blood flow and narrowed areas. Non-invasive, it is the first-line examination to be performed. It allows for the assessment of the condition of all arteries in the lower limbs and the quantification of the degree of stenosis.
Angio-CT scan or vascular MRI
to accurately map the lesions before surgery. Lower limb CT angiography, if renal function allows (iodine must be injected to perform a CT angiography) is the examination of choice for the vascular surgeon;
Important message
Any suspicion of a TIA or stroke constitutes a medical emergency. In case of sudden weakness in a limb, facial drooping, slurred speech, or sudden vision loss, emergency services must be called immediately by dialing 15. (Do not go to your doctor’s office, as this may result in a waste of time).
Some sources:
November 21, 2025N Engl J Med 2026;394:219-231DOI: 10.1056/NEJMoa2508800VOL. 394 NO. 3Copyright © 2025
