Chronic pelvic venous insufficiency: from complaint to targeted management
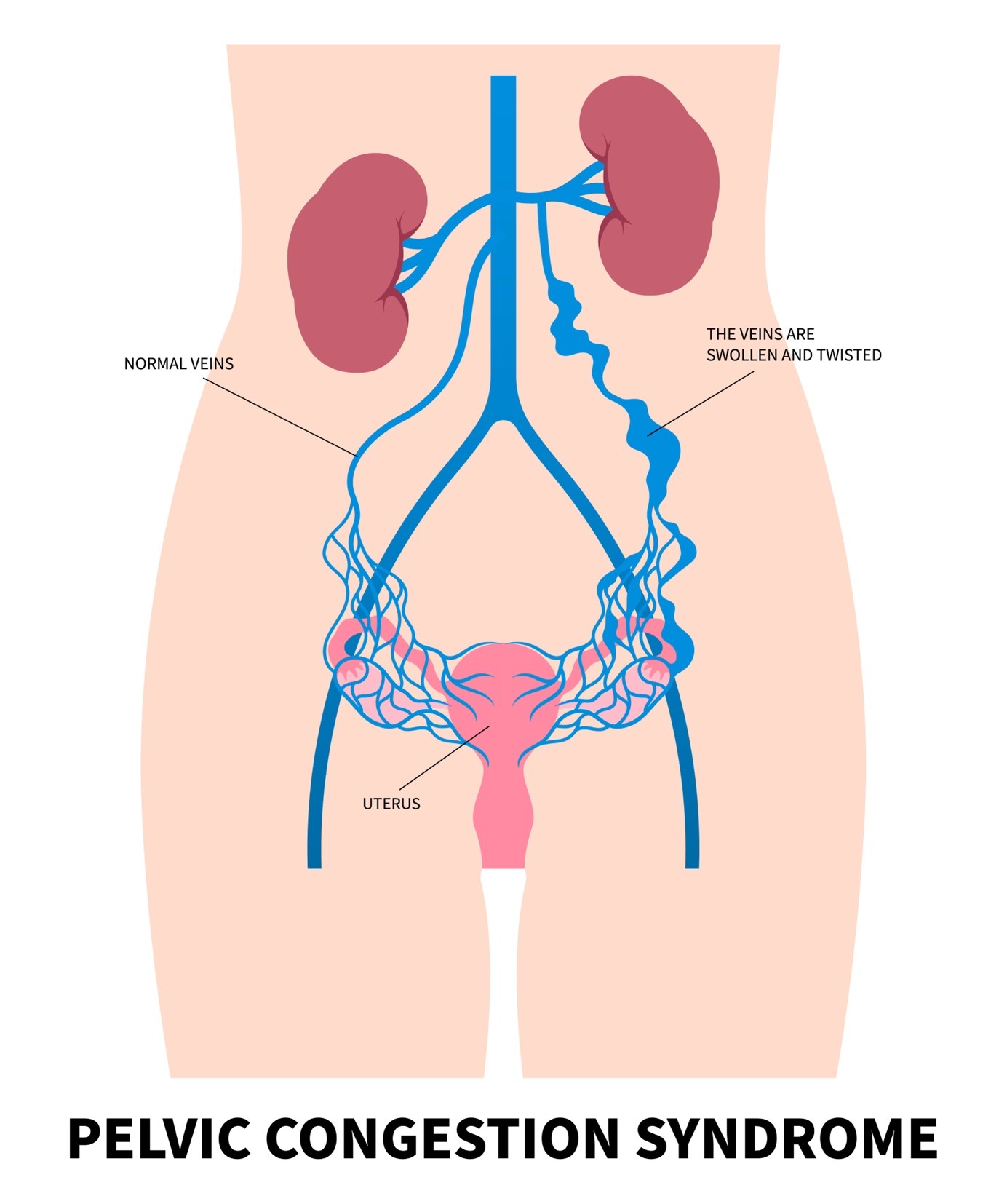
Chronic pelvic venous insufficiency (CPVI) is a common but still underdiagnosed cause of chronic pelvic pain, dyspareunia, and perineal or lower limb varicose veins of non-saphenous origin (the varicose veins do not originate from the veins of the lower limb).
It corresponds to a reflux or obstruction of the pelvic venous network, in particular the ovarian and internal iliac veins, or even to iliac-caval or reno-caval compression (such as aortomesenteric or May-Thurner syndrome).[1][2][3][4][5]

Diagnostic algorithm
- Simple organizational chart:
Step 1: clinical (pelvic pain, perineal/MI varicose veins, dyspareunia). - Step 2: Doppler ultrasound.
- Step 3: MRI / CT scan if IVPC is suspected.
- Step 4: Phlebography + endovascular procedure if symptoms are severe or resistant.
Conservative treatment: first step
Conservative treatment remains a first-line option for patients with few symptoms, in the recent postpartum period, or while awaiting interventional management.[4][8][3]
- Venous compression (shorts or tights for pelvic and lower limb compression).[8][4]
- Drug treatments: NSAIDs, progestins (e.g., medroxyprogesterone acetate), GnRH analogues, or contraceptive implants in certain situations, to reduce congestion and pain.[4][8]
- Hygienic and dietary measures: weight control, regular physical activity, adaptation of prolonged positions, management of triggering hormonal factors.
These measures may be sufficient for some patients, but high-quality evidence remains limited, and severe symptoms warrant interventional treatments.[8][3]
e
Endovascular treatments: embolization and stenting
For highly symptomatic patients, embolization of pathological pelvic veins and, if necessary, correction of iliac or renal venous obstruction now constitute the core of treatment.[7][9][2][5][3]
Embolization of the ovarian and internal iliac veins
Endovascular embolization has become the standard treatment for symptomatic pelvic venous reflux, supported by recent recommendations from learned societies (AVF, ESVS).[2][5][3]
- Venous access (often jugular or femoral), selective catheterization of the ovarian and internal iliac veins under fluoroscopy.[9][10][7]
- Embolization with coils (sometimes associated with sclerosing agents or plugs) until complete occlusion is achieved and reflux disappears.[10][7][9][3]
- It is possible to supplement this treatment with sclerotherapy of the vulvar and perineal networks or with phlebectomies of superficial escape varicose veins.[7][3]
Clinical series report an improvement in pelvic symptoms in 80–90% of cases in the medium term, with low morbidity.[5][2][3][7]
Iliac stenting and treatment of compressions
When PCIV is associated with significant iliac venous obstruction (May-Thurner syndrome) or renocaval compression, simple embolization may not be sufficient.[2][3][5]
- Placement of an iliac vein stent in cases of hemodynamically significant stenosis and severe symptoms.[10][3][5][2]
- Depending on the series, a sequential strategy is often preferred: correction of the obstruction (stent) then complementary embolization if symptoms or reflux persist.[5][2]
Studies show that normalizing abdominal, pelvic and lower limb venous flow significantly improves the quality of life of these patients.[3][5]
In summary
The vascular surgeon plays a central role in the management of chronic venous insufficiency and pelvic varicose veins. Once diagnosed, treatment is most often carried out on an outpatient basis, allowing for rapid, effective, and minimally invasive care.
Managing pelvic varicose veins and chronic pelvic congestion syndrome requires specific expertise in venous pathology. Dr. Guilhem Seban, a vascular surgeon in Annemasse, Haute-Savoie, provides diagnosis, monitoring, and treatment for these conditions, offering solutions tailored to each patient.
Sources:
[1] ASCP – Pelvic Congestion Syndrome Association: https://www.info-congestionpelvienne.fr
[2] Choosing the Most Appropriate Treatment Option for Pelvic Congestion: https://pmc.ncbi.nlm.nih.gov/articles/PMC8175116/
[3] Approach to pelvic venous disorders: https://pmc.ncbi.nlm.nih.gov/articles/PMC12668390/
[4] Pelvic Congestion Syndrome: https://www.gyneco-online.com/imagerie/le-syndrome-de-congestion-pelvienne
[5] Optimal management of combined iliac vein stenosis and ovarian vein reflux: https://www.phlebolymphology.org/optimal-management-of-combined-iliac-vein-stenosis-and-ovarian-vein-reflux-in-patients-with-pelvic-venous-disease-pevd-which-patients-should-be-treated-for-both-and-what-comes-first/
[6] Embolization of pelvic varicose veins: https://www.radiologie.fr/pratiques-professionnelles/sfr-actu/embolisation-des-varices-pelviennes-pour-traitement
[7] Pelvic venous insufficiency in women: https://medecin.veinsurg.com/case_study/insuffisance-veineuse-pelvienne-chez-la-femme-presentant-des-varices-perineales-correlation-atomo-clinique-traitement-par-embolisation-et-resultats-31-cas/
[8] Pelvic venous disorders – MSD Manuals: https://www.msdmanuals.com/fr/professional/gyn%C3%A9cologie-et-obst%C3%A9trique/troubles-menstruels/troubles-veineux-pelviens
[9] Embolization of pelvic varicose veins: https://www.radiologie-interventionnelle.fr/embolisation-des-varices-pelviennes/
[10] Embolization and Stenting for Pelvic Congestion Syndrome: https://vascular.harleystreet.sg/vascular-procedure/embolization-and-stenting-for-pelvic-congestion-syndrome/
[11] Persistent pelvic pain after embolization: https://www.american-hospital.org/traitement/douleur-pelvienne-persistante-apres-embolisation-des-varices-pelviennes
[12] Pelvic varicose vein embolization Annecy: https://radiologie-interventionnelle-74.cimdulac.fr/embolisation-des-varices-pelviennes-et-des-points-de-fuite-pelviens
[13] CLARIVEIN OC INFUSION CATHETER: https://www.has-sante.fr/upload/docs/evamed/CNEDIMTS-7159_CLARIVEIN_OC_INFUSION_CATHETER_5%20septembre%202023_7159_avis.pdf
[14] Embolization of the pelvic veins: https://www.riviera-imagerie.fr/page/embolisation-des-veines-pelviennes/
[15] European Society for Vascular Surgery: https://www.sciencedirect.com/science/article/abs/pii/S2542451322004047
